Lawmakers in several states are seeking to expand workers compensation cancer presumptions for firefighters, pointing to research linking firefighting activities with more types of cancer, and the latency period for cancer development.
Since the beginning of 2023, numerous states filed legislation that would either expand the types of cancers considered presumptive occupational injuries for first responders such as firefighters, expand the pool of covered first responders, or both.
While lawmakers are addressing cancer in first responder comp, industry researchers are also examining the issue. The Florida-based National Council on Compensation Insurance issued a report last month highlighting cancer and other presumptive occupational injuries in workers comp among firefighters and other first responders.
Firefighters are considered high risk for cancer due to workplace exposure to carcinogens, including toxins from fires, diesel fumes from idling vehicles and chemicals from firefighting gear, according to the American Cancer Society.
It’s why presumptions for firefighters suffering from cancer are increasingly common, and an annual topic for state and federal lawmakers going back to 2001, experts say.
“If it hadn’t been for 9/11, we’d probably still be fighting this battle,” said Terrence Hannigan, general counsel to the Firefighters Association of the State of New York, which represents volunteer firefighters. Numerous first responders in lower Manhattan developed lung cancer or other cancers after the attacks, which in some cases were alleged to have been linked to their exposure to toxic debris at the site of the Twin Towers.
In December 2022, President Joe Biden signed into law the Federal Firefighters Fairness Act, which created the presumption for federal firefighters.
In January, Virginia lawmakers introduced Senate Bill 906, which would add thyroid and bladder cancers as presumptive cancers for firefighters in comp.
Other states that have introduced similar first responder presumption legislation since the start of the year include, but are not limited to, Missouri, Montana, Nebraska and New Hampshire.
In January, Nebraska lawmakers introduced a bill making cancer an occupational disease for firefighters and New Hampshire lawmakers filed similar legislation stating that all types of cancers would be recognized as presumptive diseases for firefighters.
Also in January, a bill was filed in Missouri that would add more cancers to the list of presumptive diseases for many different first responders.
And in March, Montana legislators filed a bill that would add cervical cancer after 15 years, lung cancer after four years, and testicular cancer after 10 years as presumptive occupational diseases for firefighters.
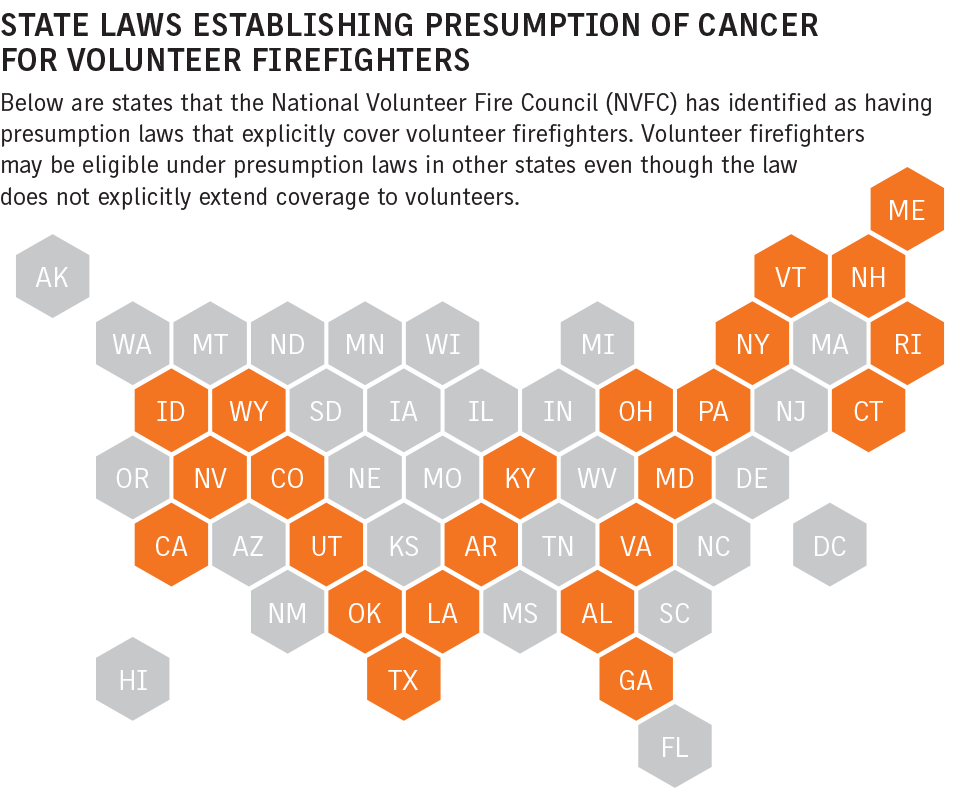
Existing state presumptions vary — more than two dozen states have them in place in some form — and not all who fight fires qualify and not all types of cancers are included. State legislatures have been working to expand benefits to volunteer firefighters (see related story).
In Pennsylvania, cancer presumptions were pushed hard for years by career firefighters, but it was volunteers who “drove it through” given the “significant political clout” held by volunteer departments, said Paul Leonard, retired manager of Upper Dublin Township, Pennsylvania and a longtime volunteer firefighter.
As manager, Mr. Leonard was aware that expanding cancer presumptions could mean increased claim activity and higher employer costs, and he worried about expanding presumptions for volunteers.
But claim costs didn’t materialize as envisioned, he said.
“It was not as bad as I originally thought,” Mr. Leonard said, adding that most of the comp cancer claims were filed by career firefighters.
Paul Cornell, director of trusts for Harrisburg, Pennsylvania-based PennPRIME, a Pennsylvania municipal insurance pool, though, said presumptions have led to increased claims and higher costs. Insurers traditionally opposed expanding cancer presumptions because of employer cost and because there was “no clarification for non-fire related cancers,” he said.
It is considered difficult for employers to rebut firefighting cancer presumptions due to a 2018 Pennsylvania Supreme Court decision that created a high employer burden for rebuttal (see related story).
Pennsylvania State Sen. Frank Farry, who was majority chair of the Fire and Emergency Services Caucus during much of his career in the state House of Representatives, sponsored a firefighter cancer presumption bill that was vetoed by former Gov. Ed Rendell in 2010. Similar legislation was signed by Mr. Rendell’s successor a year later.
Colleen Kopp, who was Mr. Rendell’s secretary of legislative affairs at the time, said the governor opposed the measure because of financial concerns.
“You couldn’t put a fiscal note on how much this legislation would cost local governments,” Ms. Kopp said. “They would be the ones who are paying these claims in their insurance policies.”
Mr. Farry said there’s no denying cancer is linked to firefighting: “These things aren’t random.”
Many synthetics found in common household items can cause fires to burn hotter and faster, “but they also put out a lot more toxins,” he said.
Bruce Spidell, actuarial committee liaison with the Boca Raton, Florida-based National Council on Compensation Insurance, said cancer presumptions for firefighters vary by state, with some listing specific presumptive cancers and others including cancer generally.
“The exact way it’s going to be rebutted will differ by state,” he said. “Every state is unique.”
Mr. Spidell, who coauthored a report in February about firefighting and first responder comp benefits, said medical research “kind of conflicts with itself” as far as what causes different types of first responder cancers.
“I think the data’s still a mixed bag, which is one of the difficulties we cited,” he said.
“Presumptions probably started out with firefighter cancer and many states have expanded it to different first responders and different diseases besides cancer,” Mr. Spidell said.
Greg Jakubowski, a fire protection engineer with Breinigsville, Pennsylvania-based infrastructure and logistics company Buckeye Partners LP, said one possible reason for the recent increase in comp cancer presumptions could be per- and polyfluoroalkyl substances, or PFAS.
The toxic compounds have been found in firefighting foam and protective gear, and many in the fire service believe increased cancer rates could be due to years of working with the chemicals.
“People didn’t know about the hazards of the foams potentially causing cancers,” Mr. Jakubowski said.
Litigation over the foam is playing out in federal court, with numerous injury suits consolidated into one multidistrict litigation docketed in South Carolina.