Several states are taking steps to address shortages of qualified mental health professionals in workers compensation by making it simpler for licensed clinical social workers to help injured workers.
California enacted a law in 2022 clearing the red tape for licensed clinical social workers to treat in the workers compensation system, and New York, after passing a law in 2020 that cleared some hurdles, is considering legislation that would modify the requirements.
Maryland lawmakers for the second year in a row are considering a bill that would allow licensed clinical social workers to treat injured workers. Under existing law, Texas allows licensed clinical social workers to assist with vocational rehabilitation.
The term social worker is often misinterpreted, which may explain why more states haven’t caught on to the trend of letting them treat injured workers, experts say.
“When people think of social workers, they often think of case managers — those in child welfare or hospitals, or helping with applications for various services,” said Sarah Hathaway, a Grand Rapids, Michigan-based licensed clinical social worker and director of behavioral health for Axiom Medical Consulting LLC, which provides services for the comp industry.
“We do all of that. But social work is a much broader field,” she said. “We can diagnose and provide therapy. With the field approaching 200,000 nationwide, social workers are critical to improving access to treatment.”
Mark Debus, Chicago-based clinical manager of behavioral health with Sedgwick Claims Management Services Inc., said the move toward permitting licensed clinical social workers to treat under workers comp makes sense, as they can manage many of the same issues typically handled by psychologists.
“Licensed clinical social workers have as much post-graduate experience as licensed psychologists in New York,” he said. “They have to meet a certain level of supervised clinical expertise, basically, and direct treatment. It’s similar to that of the licensed psychologist requirement.”
California is another state where many of the requirements for both fields are similarly stringent, according to Marcia Schwartzman Levy, a Larchmont, New York-based licensed clinical social worker in private practice and past president of the New York chapter of the National Association of Social Workers. Both states have “some of the strictest requirements for becoming a licensed clinical social worker,” she said.
Ms. Schwartzman Levy spent much of her career working in public hospitals in New York, including as a trauma unit clinical supervisor. The connection between physical injury and mental injury has been well-established, she said, pointing to literature going back to 2001 regarding injuries and the “biopsychosocial model,” a term now widely used in workers comp circles.
“I deal with bereavement, which is not just bereavement of death in the larger sense; loss of function is a form of bereavement,” Ms. Schwartzman Levy said, adding that linking mental issues and physical injuries has long been a part of what licensed clinical social workers are called on to do. “The biopsychosocial model is at the core of our belief system and training,” she said.
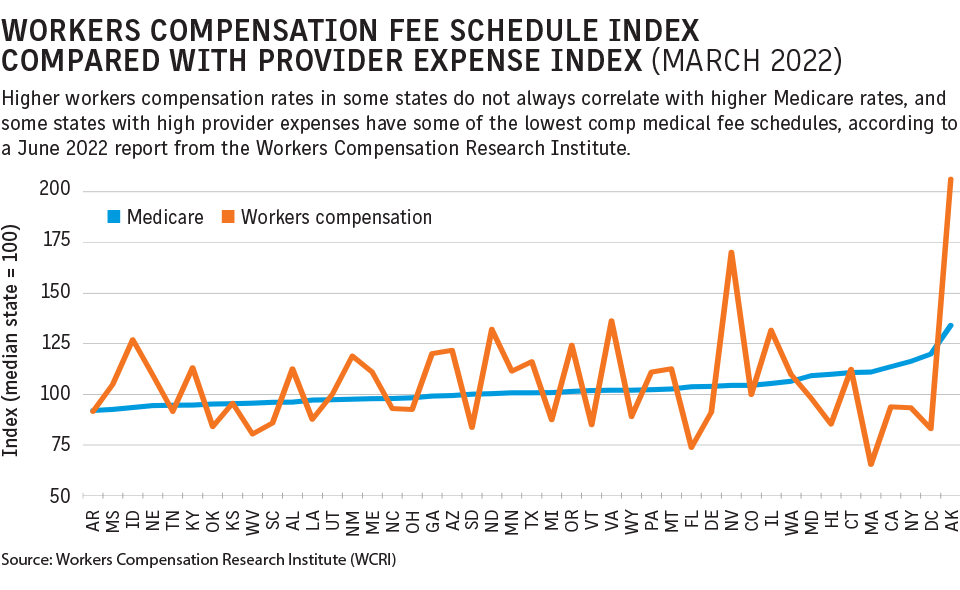
A major difference in the professions of licensed clinical social worker and psychologist is pay. “Just look at the fee schedules,” said Mr. Debus, who called social workers “underpaid.”
The Centers for Medicare and Medicaid Services’ fee schedules, on which many workers compensation fee schedules are based, has clinical social workers’ reimbursements at 75% of what is paid to a psychologist, according to a 2021 report by the National Association of Social Workers.
Jennifer Cogbill, Frisco, Texas-based senior vice president of GB Care with Gallagher Bassett Services Inc., said many psychologists are unwilling to work at the Medicare rates, which has led to a shortage of medical professionals in the workers comp field. Licensed clinical social workers could help make services more available to injured workers, she said.
“The advantage is there is a wider network of professionals they can tap into,” she said.