The cost of litigating workers compensation claims remains a concern in the industry, but there have been few court rulings overhauling costs and limited legislative efforts on the issue of attorneys fees.
One recent case in New Jersey, however, has attracted attention.
In December, a New Jersey appellate court reversed an attorneys fee award in a case brought by an injured golf course worker.
The panel said a judge erred in approving the large fee award since considerations of reasonableness, and not a blanket 20% of the award, should have been the guiding factor, even though 20% attorneys fees are permitted in New Jersey.
In this case, the attorneys representing the injured worker were awarded 20% of the $164,577 award on the permanency aspect of the case, which amounted to $32,915 in fees.
Permanency in New Jersey deals with the loss of bodily function. Medical bills and lost wages make up the other aspects of comp in the state.
The judge also awarded claimants attorneys fees of $78,000 on temporary disability benefits and medical benefits, bringing the total fees to $110,915. The appeals panel reversed the awards.
Garzon v. Morris County Golf Club was not precedential, so comp judges are not bound by it, but it generated interest, according to legal experts.
“It’s going to be discussed in the legal community,” said comp defense attorney John Geaney, co-chair of the workers compensation practice at the New Jersey law firm Capehart Scatchard, PA. “It’s something that other judges might look at. It’s persuasive.”
The awarding of attorneys fees in comp cases varies between jurisdictions, though caps are similar in many states. Many hover around 20% of the total award, although payment responsibility varies and most are contingency agreements.
In New Jersey, defendants pay 60% of attorneys fees in cases that settle, with the other 40% coming out of the total award, according to Richard Rubenstein, managing partner of Livingston, New Jersey-based Rubenstein, Berliner & Shinrod LLC.
In some states the entire fee is deducted from the injured worker award.
“The judge in Garzon failed to make a distinction between a contingency case and an hourly case,” Mr. Rubenstein said.
“We’re not allowed to charge hourly,” he said. “We’d be committing an ethical infraction. They’re asking us essentially to keep our hours when we can’t charge for them.”
Can legislation help clarify matters? Some experts are not sure there’s enough movement.
Laura Kersey, executive director of regulatory and legislative analysis for the Boca Raton, Florida-based National Council on Compensation Insurance, said the organization has tracked approximately 60 bills addressing this topic in the past five years. Few have been successful.
This legislative session only two states so far have introduced bills addressing attorneys fees.
In Tennessee, House Bill 82 would cap fees at 20% of the first 450 weeks of an injured worker’s award.
New York Assembly Bill 337 includes a revision of what claimants attorneys can submit as a claim for legal services connected to medical treatment.
Judges in various jurisdictions have also ruled on the attorneys fees issue.
Adam Levell, senior legal counsel for NCCI, said that since 2018 the council has reported on 13 cases decided by judges in nine states, with varying outcomes.
In California, there have been “a number of cases to determine the value of the attorneys’ work,” said Alan Gurvey, a Sherman Oaks, California-based applicants attorney with Rowen, Gurvey & Win. There hasn’t been “any real headway in many years in increasing fees for the applicant attorney,” he said.
California stands out from other states in that claims administrators are required to pay the fees of claimants attorneys if the defense conducts the worker’s deposition, said Sara Widener-Brightwell, general counsel for the California Workers’ Compensation Institute. Those fees are set at about 15%, according to Mr. Gurvey.
“That is probably fairly unique to California,” Ms. Widener-Brightwell said.
Kaitlyn Files, a claimants attorney running a practice in Levittown, Pennsylvania, said one controversial case in Pennsylvania was Neves v. WCAB (American Airlines), a 2020 appeals court decision determining claimants attorneys can be awarded a 20% fee on medical benefits in comp cases in addition to the wage loss portion.
What the decision left open for interpretation is who will pay the medical portion, since claimants attorneys fear it may be the responsibility of the injured worker, she said.
“There’s been somewhat of an upheaval in how each specific law firm would choose to address this issue,” Ms. Files said.
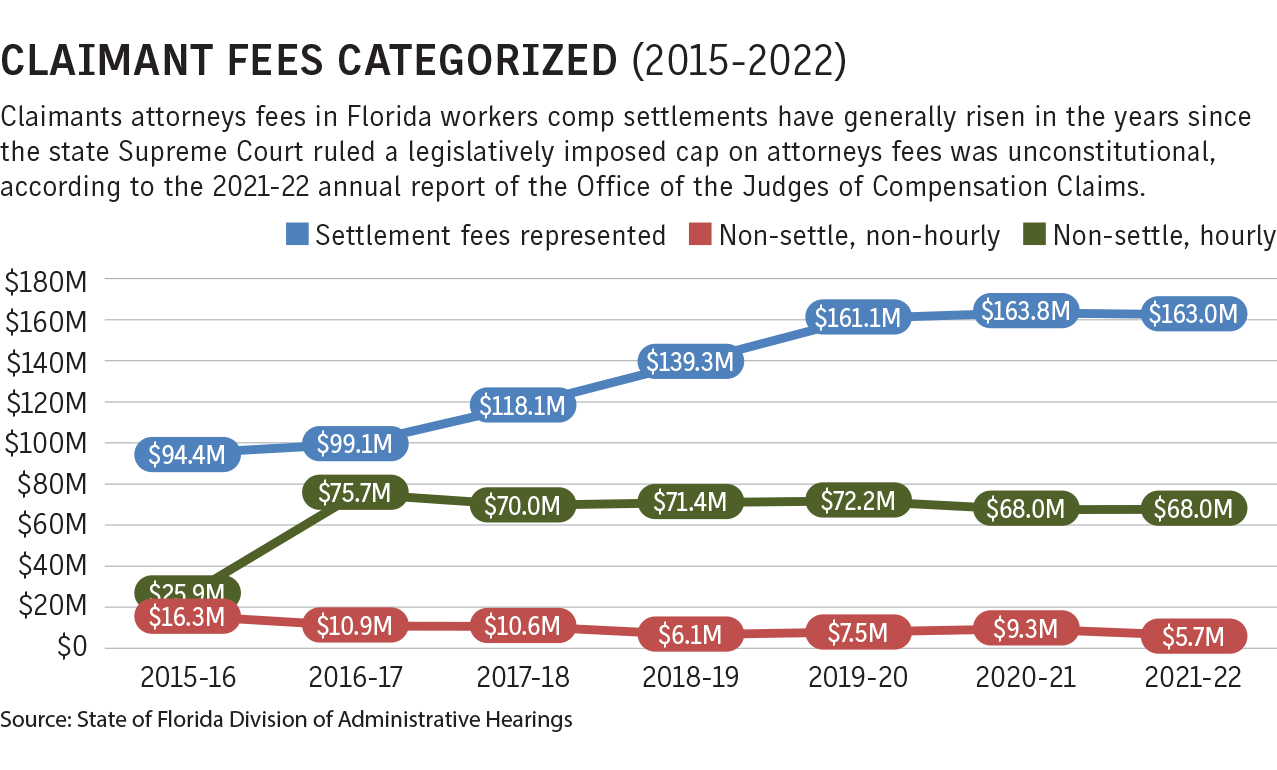
In Florida, the comp sector continues to experience confusion over the attorneys fee cap issue following court rulings, according to legal experts.
“Some judges think there is no fee cap, some judges think the word ‘reasonable’ is the fee cap, and some judges think there is a fee cap,” said David Langham, Florida’s deputy chief judge of compensation claims. “We don’t know the answer.”
The confusion stems from the 2016 Florida Supreme Court case of Castellanos vs. Next Door Co., a ruling that threw out statutorily imposed fee caps.
The decision brought back a previous system of awarding reasonable attorneys fees via judicial approval, not through statutes enacted by legislators.
Court decisions bar some state legislatures from capping charges
Some states limit what legislatures can do with regard to attorneys fees.
In 2020, a Florida workers compensation judge approved a more than $1 million attorneys fee award in a case involving a worker who had suffered brain injuries.
The fee, a little more than 25% of the total $3.9 million award, drew attention due to its size.
The award came four years after the Florida Supreme Court ruled in Castellanos v. Next Door Co. that the state’s statutory cap on attorneys fees was unconstitutional.
Justices determined fee caps should be decided by the judiciary, not legislators.
“My understanding is that it is uncapped as of this moment,” George Townsend, a Virginia-based attorney and president of the Workers’ Injury Law & Advocacy Group, said regarding Florida.
Similarly, he said, Alabama and Utah also eliminated statutory fee caps because of court rulings that reached a similar conclusion.
In 2016, the Utah Supreme Court, in Injured Workers Association of Utah v. State of Utah, found that the judiciary, not the legislature, could regulate the practice of law, including setting attorneys fees.
The Alabama Supreme Court issued a similar decision in Nora Clower v. CVS Caremark Corp. the following year.
In Florida, the Castellanos ruling initially resulted in a proposed 14.5% workers comp insurance rate increase and caused issues for employers, said Carolyn Johnson, vice president of government affairs for the Florida Chamber of Commerce in Tallahassee.
“(Employers) definitely see the upward pressure that having uncapped attorney fees has had on the system,” she said.
Ms. Johnson said work has been done to try and recap attorney fees legislatively, but “we just have not been able to do that.”