Implementing advanced technology and frontline patient advocacy are neck and neck among the fastest-growing trends in workers compensation claims management, but the best results for patients often come from balancing the two, experts say.
Improved access to data and more efficient communication should not be allowed to sterilize the claims management process, they say.
By combining technology and a personal touch, claims managers can improve care and reduce the number of litigated claims.
According to Chicago-based Rising Medical Solutions Inc.’s 10th annual benchmarking survey of claims executives, 78% of high-performing claims management organizations used one or more technology-based strategies to help injured workers in 2022, compared with 42% in 2019. The medical cost containment company surveyed 388 claims executives.
Rising’s survey also pegged “soft skills” such as empathy and listening among the top trends for organizations (see related story below).
Technology is being incorporated throughout the workers comp claims process, said Rich Ives, Hartford, Connecticut-based vice president, business insurance claim, at Travelers Cos. Inc.
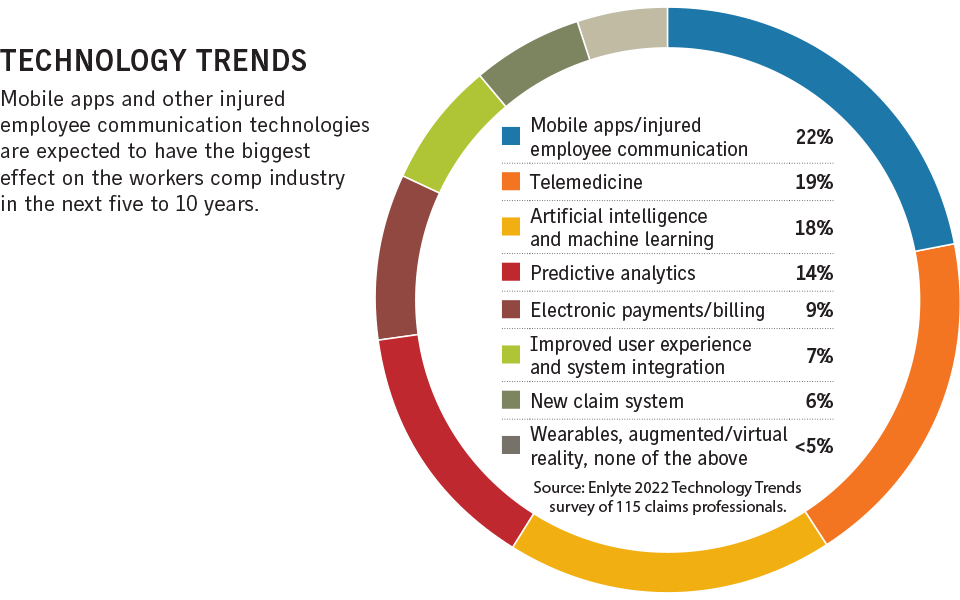
“You’ve got technology now that’s coming along, whether you’re talking about digital apps, self-service tools, analytics, predictive modeling, artificial intelligence — you name it,” he said.
Some experts have questioned whether the widespread introduction of technological tools is at odds with the emphasis on a more personal approach to claims management.
“We would say, absolutely not,” Mr. Ives said. “We call that the difference between art and science; science being more on the technology side and art being on the application of personal skills to both engage with the injured employee and to take that personalized level of care and approach. Success lies in the ideal blend of both of those things.”
Automation in workers comp has helped free up claims professionals, who were previously saddled with mundane tasks, said Jeff Gurtcheff, Lawrenceville, Georgia-based vice president, enterprise comp services, at CorVel Corp.
“Artificial intelligence is about returning time back to the claims professional so they can do those things that need the time to collaborate, communicate, show empathy, show compassion and be strategic,” he said. “We want to keep the human in the middle of this process.”
Alex Sun, CEO of Enlyte LLC, which provides workers comp services, said one of the main goals in workers comp is to shorten recovery time and speed return to work.
“That’s exactly what AI is built to do — save time and provide decision support,” he said.
Technology-based tools such as predictive modeling allow claims organizations to compare claim outcomes based on similar data points, such as age, comorbidities and other risk factors, that could impede recovery. From there, claims managers can better help injured workers who meet a certain profile and better engage with them, experts said.
Both trends help “produce a better outcome and solve challenges that we’ve not yet been able to solve,” Mr. Ives said.
Mr. Sun said technology helps organizations prioritize resources. “The more we can expedite claims processing, the more we can get information where people need it. Empowered claims professionals (can) provide personal support where it’s needed most,” he said.
Mistakes are made when “people think the technology is an end instead of a means,” said Jason Beans, CEO of Rising.
Technology “initiates a personal conversation. … The caring and the empathy that comes from a human conversation should continue, person-to-person, when that automated step initiates a response,” he said.
Mr. Ives said technology helps align resources that are going to be most valuable within the claims process. “It’s right time, right claim, right resource,” he said.
Technology’s ability to provide on-demand claim information and improve everyday communication also reduces the likelihood of litigation in claims, experts said.
Mr. Gurtcheff said cases often end up in litigation “because the communication process breaks down … because somebody feels that they can’t keep up or manage the desk effectively.”
Empathy essential as organizations boost skills to manage comp claims
The use of “soft skills” such as empathy and active listening is fast becoming vital for companies that want to successfully manage workers compensation claims, according to a recent survey of claims organizations with higher-than-average claims closure rates.
“It’s a change of culture and kind of a change of paradigm,” said Paige McCraney, vice president of care management and a nurse practitioner at Rising Medical Solutions Inc., which conducted the survey.
Sixty percent of high-performing claims organizations have implemented the so-called “advocacy model,” according to the survey results released in September.
“Historically (in workers comp) we’re looking for fault,” Ms. McCraney said. “And it’s very easy to say, ‘Oh, well, this person has mental health issues and that is really their fault.’ or ‘That’s not related to the workers comp issue,’ when it actually is caused by the workers comp injury and certainly impacts (the claim) and needs to be addressed.”
Successful claims managers are “connecting with people in a meaningful way,” said Denise Algire, Pleasanton, California-based director of health for grocery chain Albertsons Cos. Inc., who served on the advisory council for Rising’s study.
“We’re working with an injured worker dealing with what could be their worst day. Most people … don’t understand the system, and our system can be quite complicated,” she said.
In the past, the workers comp industry avoided managing the mental side of claims out of fear insurers and employers would cross into the mental-injury space and create a “psych claim,” said Dr. Marcos Iglesias, Hartford, Connecticut-based vice president and chief medical director at Travelers Cos. Inc.
But there’s a difference between having a diagnosable mental health condition and having stress, depression or anxiety when dealing with a physical injury suffered at work and not being able to work as a result, he said.
“We have lumped all of mental health into one monolith, and mental health isn’t a monolith. … Mental health is really a continuum,” Dr. Iglesias said. “At any one point in time, I might be excelling, thriving, or I might be in a crisis, and those are two very different ends of the continuum.”
Acknowledging an injured worker’s concerns, mental or otherwise, is the approach of successful claims handlers, Dr. Iglesias said.
The change is a slow process, Ms. Algire said.
“You can’t just get training on empathy. It has to be the ongoing messaging,” she said.